Translate this page into:
Subcutaneous Cerebrospinal Fluid Pseudocyst: An Unusual Complication of Ventriculoperitoneal Shunt
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Sir,
Ventriculoperitoneal shunt (VPS) is a therapeutic procedure used for the treatment of hydrocephalus of diverse etiologies. With increasing longevity following successful treatment, delayed complications are being observed more frequently. A pseudocyst is a known complication that affects patients treated with VPS. Most pseudocysts are seen in the abdomen. Rarely, a patient can have cerebrospinal fluid (CSF) collection only around shunt tube located in the subcutaneous plane and may be termed as subcutaneous CSF pseudocyst. We describe a case of subcutaneous CSF pseudocyst over chest and abdominal wall in a 12-year- male child.
A child presented with mild-to-moderate headache, gait disturbances, and progressive swelling over the anterior abdominal and chest wall for 2 months. The patient had undergone a right-sided VPS at the age of 1 year for congenital hydrocephalus. Subsequently, he underwent two revisions for shunt malfunction. Clinical examination revealed papilledema and left-sided lateral rectus palsy. Visual acuity was normal. Power was also normal in all four limbs. Local examination revealed 15 cm × 4 cm-sized elongated swelling over the anterior abdominal and chest wall [Figure 1]. The swelling appeared to be originating from the site of abdominal scar and extended upward along the course of shunt tube. A beaded appearance at the upper end of the swelling was noted. It was tense cystic, nontender, fluctuant, and irreducible. Computed tomography brain revealed dilated ventricles with periventricular lucencies. Ultrasonography revealed a cystic collection around the shunt tube with small intra-abdominal collection. The patient underwent revision of the shunt in view of shunt malfunction. A translucent cystic swelling containing clear fluid was noted in the abdominal wall coming out of the abdominal cavity [Figure 2]. The cyst was punctured and gush of clear fluid came out and the swelling subsided. The distal end of the shunt was found to be coiled and lying just beneath the abdominal wall within a small cavity. The distal slit valve was blocked and CSF was slowly coming out from proximal slit. All cultures yielded no bacterial growth. Shunt revision was carried out with good clinical outcome.
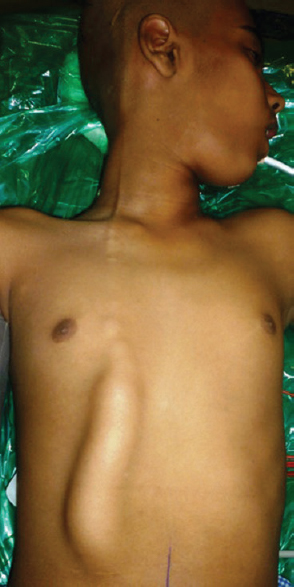
- Clinical picture showing an elongated swelling over the anterior abdominal and chest wall with a beaded appearance at the upper end

- Intraoperative picture showing the translucent cerebrospinal fluid pseudocyst
The use of the peritoneal cavity for CSF absorption in VP shunting was introduced in 1905 by Kausch.[1] In general, the shunt is made up of a ventricular catheter, a reservoir, a valve, and a long distal catheter. The distal catheter is tunneled under the skin of the scalp, neck, and chest to reach the peritoneal cavity. As more patients with treated hydrocephalus survive and live longer, more complications are being detected. The extracranial complications of VPS are classified into mechanical ones and those secondary to intraperitoneal inflammatory actions. Shunt dysfunction could be due to disconnection, obstruction, migration of the tube, or infection. The peritoneum is not the only site of CSF collection formations; cases with CSF collections have also been reported in subcutaneous cellular tissue,[2] in the breast due to breakage and migration of the distal portion of the catheter,[34] and in the neck due to perforation of the shunt after jugular catheterization.[5] Most complications are not acutely life-threatening, but they can cause shunt dysfunction and create diagnostic and therapeutic difficulties. Although the physiopathological mechanism of abdominal pseudocyst formation is unknown, predisposing factors include peritoneal adhesions from prior abdominal surgery, multiple shunt revisions, increased protein content of CSF, alterations in the absorption of CSF secondary to inflammatory or infectious processes in the peritoneum, and an allergic or nonspecific inflammatory response to the catheter.[267] CSF pseudocyst development after 35 years of shunt surgery have been describe due to local tissue reaction to shunt material. Authors concluded that extensive abdominal adhesions from previous surgical procedures predisposed pseudocyst development.[8] Hamid et al. reported four cases of abdominal pseudocyst and concluded that subclinical infection could be the probable cause.[9]
Our patient had shunt surgery at the age of 1 year. Within the next 3 months, he underwent two revisions. After that, almost for 10 years, he was asymptomatic. Hence, we do not think that abdominal wall fluid collection was due to faulty position of abdominal end of catheter outside the peritoneal cavity. Furthermore, during surgery, we have not found catheter tip into the abdominal wall cyst, so there was no reason to think that cyst resulted due to migration of catheter tip. We think that abdominal pseudocyst resulted around the shunt tip catheter. Over a period of time, this pseudocyst extended through weakened abdominal wall wound because of repeated surgery to the subcutaneous space around the shunt catheter and resulted in subcutaneous pseudocyst. The cyst was progressively increased in size and extended toward the ventricular end. Progressive decrease in size and beaded appearance over the chest were suggestive proximal flow of CSF along with the shunt tube. In the absence of catheter infection, the treatment of choice is surgical evacuation of collection and repositioning of the catheter.
Familiarity with a wide spectrum of complications arising from VPS surgery is essential for the appropriate management. Subcutaneous pseudocyst can result from multiple shunt revisions along with small abdominal pseudocyst. It can be prevented by meticulous layer-by-layer closing of the abdominal wall after putting VPS catheter into the abdominal cavity.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
- An improved technique in brain surgery: Glass tubes versus gold or platinum for subdural drainage of lateral ventricle in internal hydrocephalus. Surg Gyn Obst. 1911;13:141.
- [Google Scholar]
- Intraabdominal pseudocysts as a complication of ventriculoperitoneal shunts. J Am Coll Surg. 2003;196:297-300.
- [Google Scholar]
- Neck mass after catheterization of a neck vein in a child with ventriculoperitoneal shunt. Pediatr Neurosurg. 2004;40:182-5.
- [Google Scholar]
- Abdominal CSF pseudocysts in patients with ventriculo-peritoneal shunts. Report of fourteen cases and review of the literature. Acta Neurochir (Wien). 1994;127:73-8.
- [Google Scholar]
- Giant abdominal CSF pseudocyst in an adult patient 10 years after a ventriculo-peritoneal shunt. Br J Neurosurg. 2001;15:191-2.
- [Google Scholar]
- Abdominal pseudocyst: A rare complication of ventriculoperitoneal shunting. Pract Neurol. 2017;17:212-3.
- [Google Scholar]
- Post ventriculoperitoneal shunt abdominal pseudocyst: Challenges posed in management. Asian J Neurosurg. 2017;12:13-6.
- [Google Scholar]





