Translate this page into:
Neuroendoscopic treatment of idiopathic occlusion of unilateral foramen of Monro presenting as chronic headache
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Asymmetric ventriculomegly due to idiopathic occlusion of the foramen of Monro is rare. Such patients present with clinical features of raised intracranial pressure (ICP). Presentation as chronic headache has not been previously described. In the absence of raised ICP, pursuing surgical treatment raises a clinical dilemma as the headache may be a primary headache with no improvement after surgery. A 21-year-old woman presented with chronic headache. She was found to have asymmetric ventriculomegaly due to the occlusion of the foramen of Monro. She underwent endoscopic septostomy and widening of the foramen of Monro. Her headache subsided after surgery. At 15 months of follow-up, she was free from headache without medications. Unilateral occlusion of the foramen of Monro can present with asymmetric ventriculomegaly resulting in chronic headache. Though the symptoms of raised ICP may not be present, still endoscopic relief of ventriculomegaly leads to cure of headache.
Keywords
Foramen of Monro
foraminoplasty
hydrocephalus
neuroendoscopy
septostomy
Introduction
Unilateral ventriculomegaly is well-described in children secondary to neoplastic or infectious causes, and also due to congenital atresia, with or without the presence of a membrane.[1] Idiopathic occlusion of the foramen of Monro in adulthood is exceedingly rare, with only 14 cases previously described.[2] These patients present with clinical features of raised intracranial pressure (ICP) necessitating early treatment.[2] Neuroendoscopic septostomy and/or foraminoplasty are the treatment of choice for this condition.[134] Presentation as chronic hydrocephalus without clinical and radiological features of raised ICP poses a dilemma regarding surgical treatment. There is a possibility that the patient may have a primary headache, and imaging findings are incidental. In such scenario, the patient's headache may not be relieved with surgery. We describe a case of unilateral hydrocephalus due to foramen of Monro occlusion, presenting as chronic headache, successfully treated with neuroendoscopy.
Case Report
A 21-year-old woman presented with headache of 5 years duration. The headache used to be left-sided accompanied with vomiting, and intolerance to noise and light. The frequency of headache was 3–4 times a month. She was diagnosed with migraine headaches, and took the following drugs for migraine: Flunarizine, propranolol, tramadol, and naproxen. She had partial relief with flunarizine. However, she developed episodic retro-orbital pain with nausea. There was no history suggestive of neither prior central nervous system infection nor intraventricular hemorrhage. There was no papilledema. The neurological examination was normal throughout the course of illness. The initial diagnosis was migraine. A combination of above-mentioned drugs was tried sequentially but did not relieve headache. She was evaluated with a magnetic resonance imaging (MRI) of brain, which revealed the dilatation of left lateral ventricle, with no periventricular lucency. As she did not have any classical clinical features of raised ICP, the headache was not attributed to asymmetric ventriculomegaly. She was asked to continue medications. She underwent MRI twice at the annual interval, with no change in her ventriculomegaly. The constructed interference in steady state three-dimensional sequence revealed a membrane blocking the foramen of Monro but no lesion [Figure 1]. Lumbar puncture was not done to find the etiology of the occlusion of foramen as the patient had unilateral ventriculomegaly, and it was deemed as a contraindication. A final diagnosis of idiopathic occlusion of the left foramen of Monro was made. The proposed mechanism of headache was probably raised ICP due to obstruction of the foramen of Monro. As she did not have adequate relief of headache, a decision for surgery was taken after mutual discussion with referring neurologist and patient.
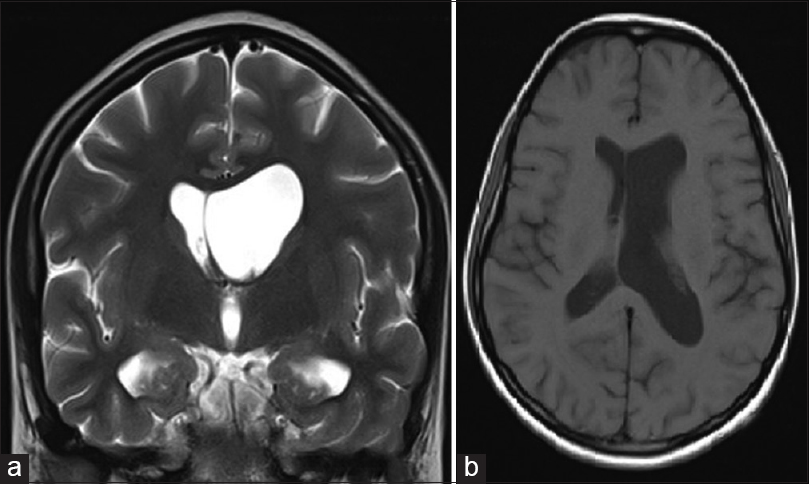
- Magnetic resonance imaging showing asymmetric ventriculomegaly and membrane at the left foramen of Monro. (a) T2-weighted coronal acquisition. (b) T1-weighted axial acquisition
She underwent left precoronal burr hole, and neuroendoscopy. As the patient had left ventriculomegaly, burr hole was placed on left side. The right side ventricle was small, and negotiation of endoscope in the right ventricle would have been technically difficult. Moreover, the aim of surgery was also to inspect the occluded foramen and dilate it if possible, hence left side approach was used. After making the burr hole a ventricular cannula was inserted, and ICP was measured by attaching it to a transducer that was connected to monitor. The opening pressure was 22 mm Hg. The endoscope was inserted after ICP monitoring for 5 min. The fenestration of the septum pellucidum was performed at the level of avascular zone, between anterior and posterior septal veins. The fenestration was done with bipolar probe without coagulation. The stoma was dilated using a Fogarty balloon no. 3. At the end of the septostomy, the endoscope was introduced into the stoma to inspect the contralateral ventricle and confirm the adequacy of septostomy. There were membranes at ipsilateral foramen of Monro which were fenestrated [Figure 2]. No attempt to widen the foramen of Monro was done. The ventricular cerebrospinal fluid (CSF) analysis was normal, hence infection was ruled out. She was discharged with instruction to take paracetamol for headache as and when required. At 3 months of follow-up, she was free from headache without medications. At follow-up of 15 months, she was still free from headaches. An MRI done at 15 months showed septostomy defect; however, the membranes at foramen Monro were persistent [Figure 3]. There was no appreciable reduction in the size of ventricle.
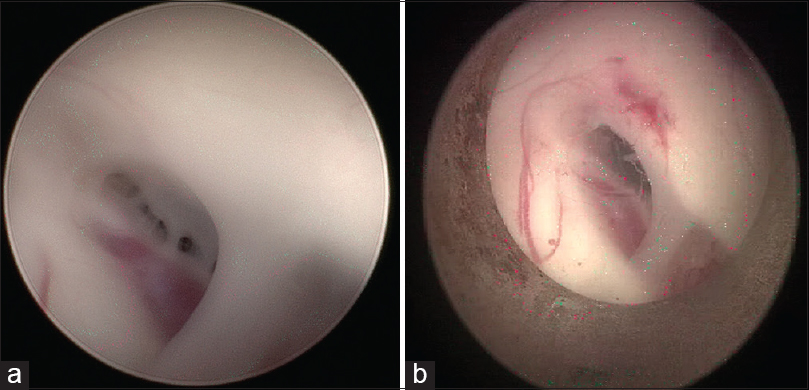
- (a) Endoscopic view of membranes at the foramen of Monro. (b) Dilated foramen after formanioplasty
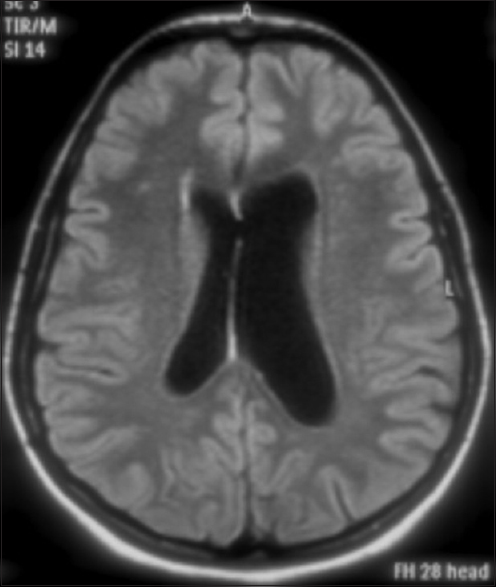
- Magnetic resonance imaging at follow-up showing patency of septostomy
Discussion
Though unilateral ventriculomegaly due to the occlusion of the foramen of Monro is described in the literature, our case is unique in terms of clinical and radiological presentation. Our patient did not have classical clinical as well as radiological features of raised ICP leading to dilemma of surgical treatment. There were no classical symptoms of raised ICP such as headache with vomiting and blurring of vision and papilledema in present case. Though raised ICP can present as chronic headache, it was difficult to ascribe headache to intracranial pathology in present case. The patient underwent MRI twice before a decision of surgery was taken. The inherent risks of procedure including bleeding and subdural hygroma were kept in mind. Hence a conservative treatment in our case was continued for few years. As her headache was not responding to medications, the option of surgical treatment was considered. After thorough and repeated discussion with patient and referring neurologist neuroendoscopy was performed. A septostomy was done to establish communication between ventricles so that CSF can drain through opposite side normal ventricle. The patient had sustained relief from headache after surgery. The relief of headache was due to normalization of ICP. Though there was no appreciable reduction in the size of ventricles at follow-up MRI, the treatment was still considered successful as the patient had headache relief. One may argue that the cause of relief of headache is not surgery as there was no reduction in ventricular size. Though comparison ventricular measurements are not available in cases of unilateral ventriculomegaly, it is known that in the cases of endoscopic third ventriculostomy, ventricular size is not always reduced. The proportion of patients who do not have ventricular size reduction ranges between 11% and 60%. The ventricular size reduction is easier to appreciate in patients with acute hydrocephalus, whereas in chronic hydrocephalus the ventricular size changes are subtler and in some cases are only perceived when detailed measurements or volumetric studies are performed. Currently, the consensus is that ventricular size reduction does not seem to correlate with clinical outcome.[5] In patients with chronic hydrocephalus, there may not be reduction in the size of ventricles after neuroendoscopic procedure, in such cases the success of treatment should be measured by clinical rather than radiological improvement.[5]
The neuroendoscopic options for unilateral occlusion of the foramen of Monro are septostomy and/or foraminoplasty.[134] Though fenestration of membranes at the foramen of Monro was done in our patient, the patency could not be established as evident by the persistence of membranes visible on MRI at follow-up. However, the patency of septostomy helped the circulation of CSF, and relief of headache. Endoscopic septostomy is safe and effective treatment for unilateral hydrocephalus. The early success rate of more than 95% and a long-term success rate of 92% has been described with septostomy.[6] The septostomy allows the obstruction to be bypassed by creating a CSF circulation between the obstructed ventricle and the opposite ventricle communicating with the third ventricle. Thus, septostomy avoids the need for ventriculo-peritoneal shunt. The same aim can be achieved by performing a foraminoplasty, but it poses higher risk of injuring the adjacent fornix, veins, and hypothalamus.[6] Unilateral hydrocephalus due to the occlusion of foramen of Monro can present with chronic headache. Endoscopic septostomy is safe and effective treatment for cure of headache in such case.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Neuroendoscopic foraminal plasty of foramen of Monro. Childs Nerv Syst. 2008;24:933-42.
- [Google Scholar]
- Adult idiopatic occlusion of monro foramina: Intraoperative endoscopic reinterpretation of radiological data and review of the literature. Br J Neurosurg. 2014;28:717-21.
- [Google Scholar]
- Idiopathic bilateral stenosis of the foramina of Monro treated using endoscopic foraminoplasty and septostomy. Neurosurg Focus. 2011;30:E5.
- [Google Scholar]
- Neuroendoscopic fenestration of the foramen of Monro without septostomy for unilateral hydrocephalus following neonatal intraventricular hemorrhage. Childs Nerv Syst. 2011;27:473-8.
- [Google Scholar]
- Functional analysis of third ventriculostomy patency by quantification of CSF stroke volume by using cine phase-contrast MR imaging. AJNR Am J Neuroradiol. 2005;26:2514-21.
- [Google Scholar]
- Endoscopic septostomy through a standard precoronal ventricular access: Feasibility and effectiveness. Acta Neurochir (Wien). 2012;154:1517-22.
- [Google Scholar]






